Pilot Hypoxia: How to Recognize and Respond to the High-Altitude Threat
“One becomes indifferent. One thinks neither of the perilous situation nor of any danger,” French balloon pilot Gaston Tissandier wrote after narrowly surviving the first documented aviation-related hypoxia event at 28,000 feet.
Regardless of what altitude we usually fly at to understand the types of hypoxia, its symptoms and effects, plus what to do if we find ourselves sliding into the dangerously peaceful grip of low oxygen levels. Let’s jump right in.

Featured Pilot Gear
Browse our selection of high-quality pilot supplies! Your purchase directly supports our small business and helps us continue sharing valuable aviation content.
“One becomes indifferent. One thinks neither of the perilous situation nor of any danger,” French balloon pilot Gaston Tissandier wrote after narrowly surviving the first documented aviation-related hypoxia event at 28,000 feet.
Many pilots want to believe that hypoxia only happens to “other people” or at “higher altitudes than I fly,” but 15% of the respondents in a 2019 Embry-Riddle general aviation pilot hypoxia survey reported experiencing symptoms at or below 10,000 feet.
When hypoxia does occur in the cockpit, it is usually deadly. Records show that 85% of the thirteen hypoxia related accidents recorded by the NTSB since 2000 have resulted in fatalities.
What’s worse, these thirteen accidents are likely just the tip of the hypoxia iceberg. The prevalence of hypoxic pilot events is unknown since commercial and general aviation pilots are not legally required to report episodes of hypoxia that do not result in incidents or accidents.
In fact, although 78% of the GA pilots in the Embry-Riddle survey reported experiencing symptoms consistent with hypoxia, 94% did not report the event.
Many of these pilots had little to no hypoxia awareness training and did not realize the symptoms they were experiencing were related to decreased oxygen levels.
Clearly it’s important for all pilots regardless of what altitude we usually fly at to understand the types of hypoxia, its symptoms and effects, plus what to do if we find ourselves sliding into the dangerously peaceful grip of low oxygen levels.
Let’s jump right in.

What is Hypoxia?
The medical definition of hypoxia is “a state in which oxygen is not available in sufficient amounts at the tissue level to maintain adequate homeostasis.” In simple terms, hypoxia is a medical condition that occurs when our cells are not receiving enough oxygen to function normally.
Types of Hypoxia
There are four main hypoxia types. Each has a different cause, but their signs and symptoms are the same. They also all have the same net result of the body not receiving the oxygen it needs to function properly.
Hypoxic Hypoxia
At higher altitudes, oxygen molecules are spaced farther and farther apart. This change in molecule spacing is measured by the pressure per square inch and is expressed as the partial pressure of oxygen.
As partial pressure decreases, it is harder for our bodies to take in and absorb enough oxygen to meet our needs. This oxygen debt causes hypoxic hypoxia.
Stagnant Hypoxia
When our blood has enough oxygen, but the flow of blood is restricted, we experience stagnant hypoxia. High G forces can shunt blood away from the brain and trigger stagnant hypoxia in fighter pilots.
When a commercial or GA pilot encounters stagnant hypoxia, it is more likely caused by poor circulation or a blocked or constricted blood vessel.
Hypemic Hypoxia
Hypermic hypoxia occurs when there is enough available oxygen entering the lungs, but there is a problem with the red blood cells that are supposed to transport the oxygen throughout the body.
Decreased blood volume from extreme bleeding or recent blood donation can increase the potential for hypermic hypoxia. Anemia, sulfa drugs, and nitrites also decrease the blood’s oxygen carrying capacity, as does smoking.
The most likely scenarios in which a pilot could experience hypermic hypoxia are through smoking or carbon monoxide poisoning. When carbon monoxide is absorbed by our bodies, it binds to the red blood cells leaving little to no room for oxygen to bind to the cells and be transported to our tissues.
Carbon monoxide poisoning could be brought on by an aircraft malfunction such as an engine manifold leak, aircraft heater problem, or exhaust infiltration into the cabin.
A carbon monoxide triggered hypermic hypoxia may be averted or addressed early by carrying a portable carbon monoxide detector in the cockpit.
Histotoxic Hypoxia
With histotoxic hypoxia, oxygen is carried throughout the body, but the cells are blocked from accepting or using it. Alcohol and narcotics are the two most common causes of histotoxic hypoxia.
Note that even if you allow the minimum required 8 hours from bottle to throttle, you could still be at a higher risk for histotoxic hypoxia than a pilot who did not have a drink.
What Type of Hypoxia Can Pilots Get?
Although pilots can suffer from any of the four types of hypoxia, the most common type of pilot hypoxia is hypoxic hypoxia.
What Happens to Pilots When They Get Hypoxic?
Hypoxia is dangerous for pilots because their ability to fly the aircraft safely and effectively degrades. Without proper oxygen levels, pilots experience slower reaction times and are prone to poor decision making, which can be fatal. Untreated hypoxia can progress to unconsciousness from which the pilot never awakens.
How High Can a Pilot Fly Without Oxygen?
FAA regulations require flight crews to be provided with and to use supplemental oxygen after 30 minutes at cabin pressure altitudes of 12,500 to 14,000 feet.
Supplemental oxygen is required immediately once flights reach a cabin pressure altitude of 14,000 feet. If the cabin pressure altitude is above 15,000 feet, everyone onboard must have and use supplemental oxygen.
This means that a pilot can indefinitely legally fly as high as 12,499 feet without oxygen. Pilots can also choose to fly up to twenty-nine minutes at a maximum altitude of 13,999 feet without violating FAA regulations.
Both these examples fall under the “just because you can, doesn’t mean you should” caveat. Most pilots will experience at least some initial effects of hypoxia below the 12,500’ threshold, especially when flying at night.
The more conservative FAA recommendation is to use supplemental oxygen above 5,000 feet at night and above 10,000 feet during the day.
At What Altitude Do You Become Hypoxic?
There is no single set altitude where hypoxia kicks in for all pilots. In the real world, the onset of hypoxia happens at different altitudes depending on each pilot’s physiology.
Hypoxia in pilots symptom onset altitude can also shift due to age, medical conditions, level of acclimatization, and other factors.
For example, a young pilot who lives in Denver and has no exacerbating medical conditions will likely experience initial hypoxia onset at a higher altitude than an older pilot from Boston who is a smoker and has an underlying pulmonary condition.
That said, most pilots will begin to experience the effects of hypoxia at pressure altitudes of between 7,000 and 10,000 feet, with some pilots having mild initial symptoms at altitudes as low as 5,000 feet. Symptom severity increases rapidly as pilots ascend above 10,000 feet without supplemental oxygen.
Why do Some Pilots Get Hypoxic at Lower Altitudes?
No one knows for sure at exactly what pressure altitude they will start to experience hypoxia symptoms, but certain non-altitude related factors can increase the potential for hypoxia at lower altitudes.
Exacerbating factors include:
|
|
How to Tell if You are Hypoxic
Rapid-onset hypoxia as in the case of sudden aircraft depressurization is easier to recognize because a dramatic event causes the hypoxia. If you lose pressure, you know to expect hypoxia and will automatically be taking steps to mitigate its effects.
Slow-onset progressive hypoxic hypoxia caused by steady altitude gain or sustained flight at higher altitudes without oxygen supplementation or aircraft pressurization is harder to recognize.
Symptoms develop and worsen so incrementally you may not even notice them until they have progressed to a point where you are too impaired to respond appropriately and effectively.
The best ways to catch slow-onset hypoxia are by learning the symptoms of hypoxia and by monitoring your oxygen levels.
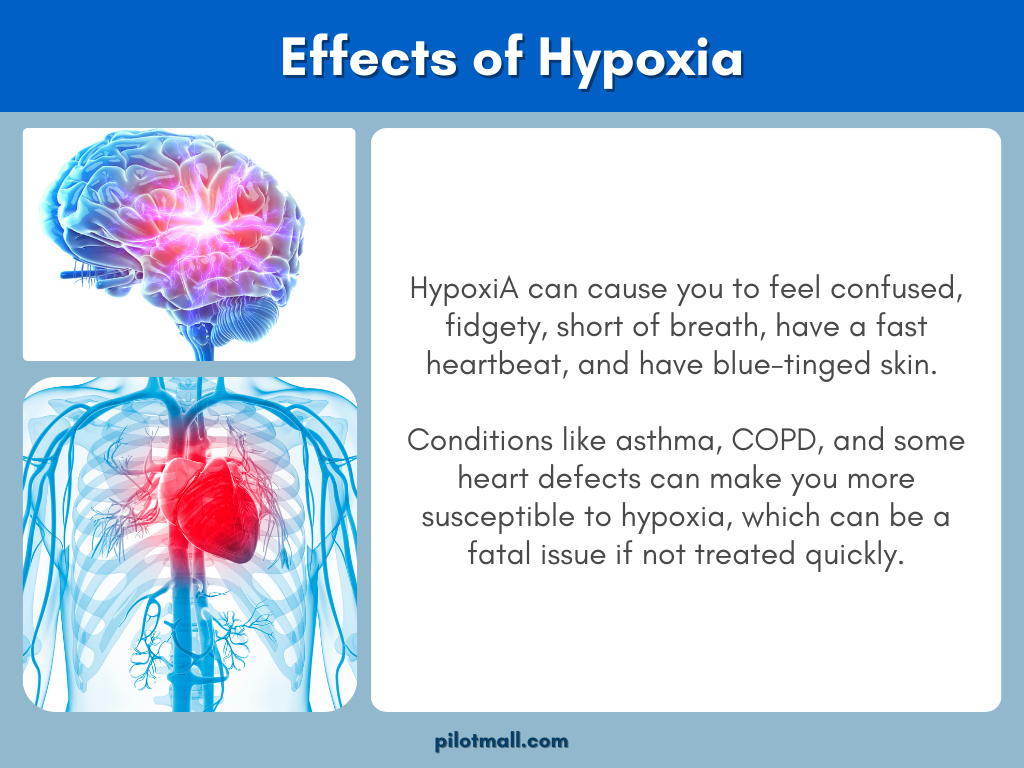
 Signs and Symptoms of Hypoxia in Aviation
Signs and Symptoms of Hypoxia in Aviation
With slow-onset hypoxic hypoxia, pilots typically experience several initial symptoms which increase in severity over time. The longer the pilot remains in a hypoxic state, the more symptoms they will experience and the worse those symptoms will get.
If steps are not taken to improve the pilot’s oxygenation levels, more severe later symptoms can develop. At this point the pilot will be rendered completely incapacitated and incapable of controlling the aircraft.
The most common initial and later symptoms of hypoxia include:
Hypoxia Signs and Symptoms
|
|
Stages of Hypoxia
Hypoxia is cumulative and if left untreated progresses through the following four stages:
Indifferent Stage
During the indifferent stage pilots do not experience any symptoms of hypoxia. Oxygen saturation percentages average 90-97%. The average altitude for the indifferent stage is 0-5,000 feet.
Compensatory Stage or Complete Compensatory Stage
Our eyes require the highest levels of oxygen, so they are the first body part to be affected by hypoxia. We experience decreased visual acuity. Colors can begin to fade, and night vision is most strongly impacted. Night vision is degraded by 10% at 5,000 feet and 30% by 10,000 feet.
When we encounter a hypoxia-inducing scenario, our bodies are designed to automatically try to maintain normal functioning. Deeper, more frequent breaths and yawning are signs of our bodies attempting to compensate for the continued decreased tissue oxygenation. Pulse rate and blood pressure also increase.
Disturbance Stage or Partial Compensatory Stage
Hypoxia symptoms are subtle during the first two stages, and if we aren’t alert, we could miss them. Once our bodies are no longer able to compensate for the reduced oxygenation, we enter the disturbance stage of hypoxia, and symptoms are more pronounced.
Euphoria is the most common initial symptom of the disturbance stage of hypoxia. This is dangerous because it can lull an unsuspecting pilot into missing the warning signs of hypoxia until it is too late to respond effectively. Other common disturbance stage symptoms include impaired judgement, drowsiness, and confusion.
Hearing is one of the last senses to be impacted by hypoxia, so pilots can still hear radio communications and verbal commands even during the later parts of the disturbance stage though they will struggle to understand and respond to anything other than simple, clear, repeated commands to apply oxygen and/or decrease altitude.
Critical Stage
Once a pilot enters the critical stage of hypoxia, they rapidly become unconscious before progressing into a coma and then death.
Pilot Hypoxia Training
Since each of us experience hypoxia onset at different altitudes and have a unique progression of symptoms, the best way to know how our bodies react to hypoxia is to experience it firsthand and take notes.
The FAA requires pilots who will routinely be flying at FL250 and higher to go through mandatory high altitude and high airspeed training which includes a segment on hypoxia. Versions of the hypoxia training are available to GA pilots as well.
The FAA offers interactive, hands on one-day aviation physiological training courses at the Civil Aeromedical Institute (CAMI) in Oklahoma City. Pilots who enroll in the in-person course get to experience altitude-induced hypoxia in a controlled altitude chamber environment.
 What to Do if You Start to Become Hypoxic While Flying
What to Do if You Start to Become Hypoxic While Flying
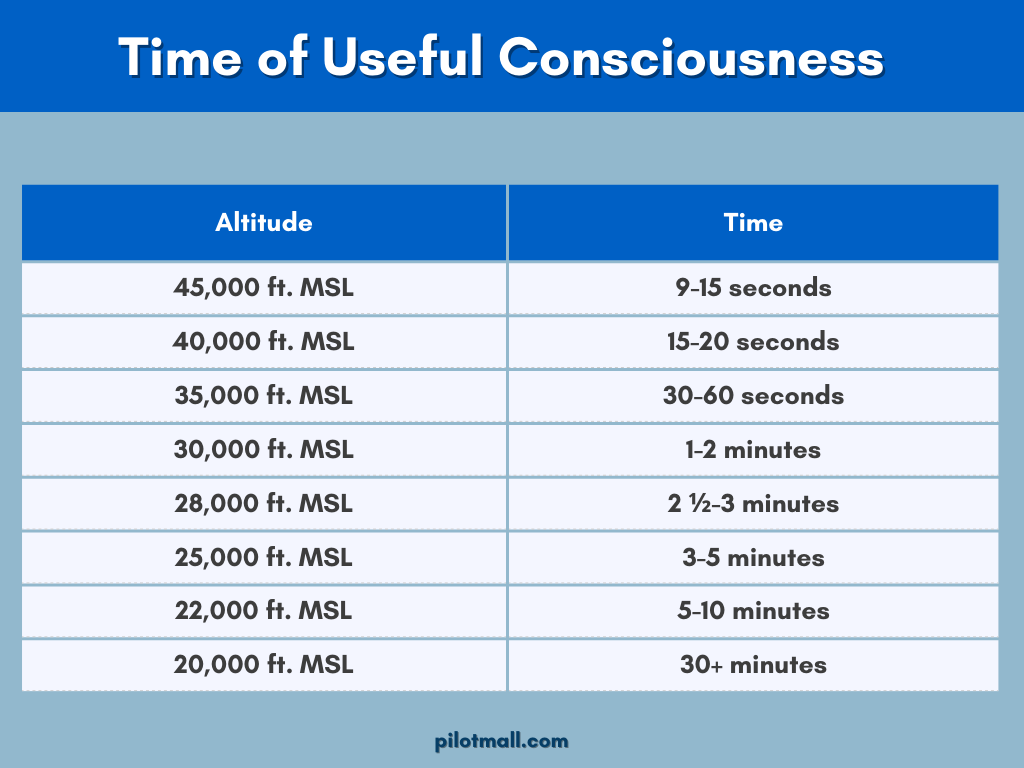
The higher your altitude, the shorter time of useful consciousness (TUC) you have available to take corrective action once you begin to experience hypoxia.
At 20,000 feet MSL, pilots have up to 30 minutes of useful consciousness. Increase your altitude just 2,000 feet, however, and your TUC decreases to 5 to 10 minutes.
The TUC continues to drop off rapidly with increased altitude and is just 9 to 15 seconds at FL450 (45,000 feet).
1. Put on your oxygen
The most important corrective action hypoxic pilots can take is to immediately apply supplemental oxygen if it is available. Remember, your condition will not improve until you increase the supply of oxygen in your blood. Just a few seconds of breathing supplemental oxygen can rapidly decrease hypoxia symptoms.
2. Check your oxygen equipment
If you were already wearing your oxygen mask when you became hypoxic, check your equipment to ensure oxygen is flowing. Make sure the tank has pressure, the regulator is open, and the tubing is not kinked.
3. Descend as soon as safely possible
Once you have applied your supplemental oxygen, safely descend to a lower altitude as soon as possible. Decreasing your altitude to 10,000 feet or lower will help raise your blood oxygen levels.
4. Ask for assistance
If necessary, contact ATC and declare an emergency. Tell the controller what happened. Depending on how advanced and extended the hypoxic event was, you may be unaware of the severity of your impairment.
A clear-thinking third party can talk you through navigating to and landing at the closest appropriate airfield.
Pilot Hypoxia Case Studies
It’s time to put what we’ve learned into action by listening to actual recordings of three pilots who experienced varying degrees of hypoxia in the cockpit. In all three of these cases, the pilots were ultimately able to safely land the aircraft.
As you listen to the pilots, note their cognitive state, level of responsiveness to the ATC controller, aircraft handling abilities, and capacity for critical decision making.
In the comments section, share which symptoms of hypoxia you noticed simply from listening to the radio traffic.
Case Study 1: Cirrus SR22 N591WA Flight from San Bernadino, CA to Colorado Springs, CO
In the onset of this incident, the pilot and his wife are flying a Cirrus SR22 aircraft at 17,000 feet. The pilot finishes acknowledging his route into Colorado Springs at time stamp 1:10 and confirms he is maintaining an altitude of 17,000.
At time stamp 4:18, the controller checks in with the pilot to ask if he has a request but there is no initial reply. Ten seconds later, the pilot finally responds.
Notice the change in his voice, breathing, and speech pattern since his initial communication at 25 seconds into the official recording and his route confirmation at 1:10.
The controller immediately recognizes signs of hypoxia and replies asking the pilot if he would like a lower altitude, however the pilot is already unable to process the question and instead keeps replying with only his call sign until timestamp 5:05. The pilot is instructed to descend to 13,000 feet at his discretion, but nearly a minute later at 5:55, he is still at 17,000 feet.
At 6:33, the pilot’s wife gets on the radio and states that she is trying to help. She does not sound like she is experiencing hypoxia. The pilot seems to have either lost consciousness or to be marginally conscious at this point. He has gone from fully coherent to completely incapacitated in less than six minutes.
The controller talks the pilot’s wife through guiding the aircraft down to a lower altitude. The pilot finally regains consciousness around timestamp 16:55 but is disoriented and still impaired.
At 18:20, the wife says the pilot is “getting there” in response to the controller asking whether the pilot is flying the aircraft. They are now flying at an altitude of 10,200 feet.
At 23:00, a full seventeen minutes after losing consciousness, the pilot is finally alert enough to respond to the controller again. Notice the residual impairment to his reasoning skills, however.
If his wife had not been in the aircraft with him and the controller had not been able to talk her through flying the aircraft, this story could have ended very differently.
When flying with passengers, do they know what to do if you are incapacitated?
Case Study 2: Kalitta Learjet KFS66 Flight from Manassas, Virginia to Ypsilanti, Michigan
The audio for this incident picks up as the pilot is flying at FL320 and has just been handed off to the Cleveland Control Center. The aircraft has had a pressurization system malfunction of some sort.
Notice the alarms blaring in the background as the ATC controller initially thinks the pilot just has a stuck mike.
The pilot manages to state that he is declaring an emergency, but he does not state the nature of the emergency. A second pilot assumes the emergency is with the flight controls and the ATC controller proceeds with that assumption until one of the pilot’s responses tips him off to the hypoxia problem. What alerts the controller to the true problem?
Case Study 3: Cessna 208B VH-DQP Flight from Cairns to Redcliffe, Queensland Australia
The pilot of Cessna VH-DQP was flying solo at an altitude of 10,000 feet when he encountered icing conditions and poor visibility due to cloud cover.
He climbed to 11,000 feet and became unresponsive on the radio for a period of 40 minutes. The pilot was later found to have fallen asleep due to a combination of fatigue and mild hypoxia.
Once the pilot wakes up and re-establishes communications, notice his repeated requests for the controller to “stand by one” in response to questions and his initial insistence on continuing to his originally planned destination airport despite having only minimal additional fuel reserves.
What lingering hypoxia symptoms do you notice after communications are restored?
Air Force Pilot Controlled Hypoxia Training
Military pilots and crew receive hypoxia training in a controlled altitude chamber. Watch as the pilot in this hypoxia training video spends just under three minutes at a simulated 25,000 feet without supplemental oxygen.
He is instructed to hold up playing cards and state the suit and number on each card plus verbalize the hypoxia symptoms he is experiencing.
Notice what happens once he reaches and surpasses his time of useful consciousness. The pilot is still conscious but how well does he complete the assigned task? What is his level of comprehension and responsiveness to the instructions of his instructor?
Once he is back on supplemental oxygen, how long does it take to notice an improvement in the pilot’s cognitive function?
How to Avoid Pilot Hypoxia
None of us want to lose consciousness while flying. As with many in-cockpit emergencies, the best way to deal with hypoxia is to educate ourselves about the risk, then take steps to minimize or avoid it altogether.
A best practice is to follow aviation risk management strategies to decrease your odds of experiencing a hypoxic event while flying.
 Use Monitoring Tools
Use Monitoring Tools
Invest in a pulse oximeter, also called an SPO2 meter to monitor your blood oxygen levels. Pulse oximeters are readily available at pharmacies, big box retailers, and online. They are one of the best ways to tell if you are becoming hypoxic.
An SPO2 meter will monitor how much oxygen is available in your blood. Unless you have a known condition that decreases your SPO2 levels, you should see readings of 95% or higher.
In an otherwise healthy pilot, any reading of 90% or lower while flying indicates a hypoxia problem that needs to be addressed.
Fly With (and Use) Supplemental Oxygen
The surest way to avoid pilot hypoxia is to outfit your aircraft with built-in or portable onboard oxygen. Step two is to then actually use said oxygen when you are flying at and above your personal hypoxia thresholds and in conditions that increase the risk of hypoxia.
Keep Building Your Pilot Safety Knowledge with These Articles:
- The Silent Killer in the Cockpit
- Aviation Risk Management (Learn from the Pros)
- 10 Ways to Fight Pilot Fatigue
Did you find this article helpful?
Do you think we missed anything important? Let us know in the comments below!